COVID-19 and mental health
For many people, the COVID-19 pandemic has introduced and increased a range of psychosocial hazards in the workplace at a time when a range of other non-work-related psychosocial risks are also occurring (uncertainty about future employment, social isolation etc.).
OSH laws cover risks to psychological (mental) health, too. This is a stressful time for all Australians, and you must do what is reasonably practicable to eliminate and reduce the psychological risks to workers and others in the workplace.
Under OSH laws, you have a duty to provide a safe and healthy workplace and to take action to prevent or minimise risks to the health and safety of employees.
What causes psychological injury? What are psychosocial hazards?
*A psychosocial hazard is anything in the design or management of work that causes stress. Stress is the physical, mental and emotional reaction a person has when we perceive the demands of their work exceed their ability or resources to cope. Work-related stress, if prolonged or severe, can cause both psychological and physical injury. Stress itself is not an injury.
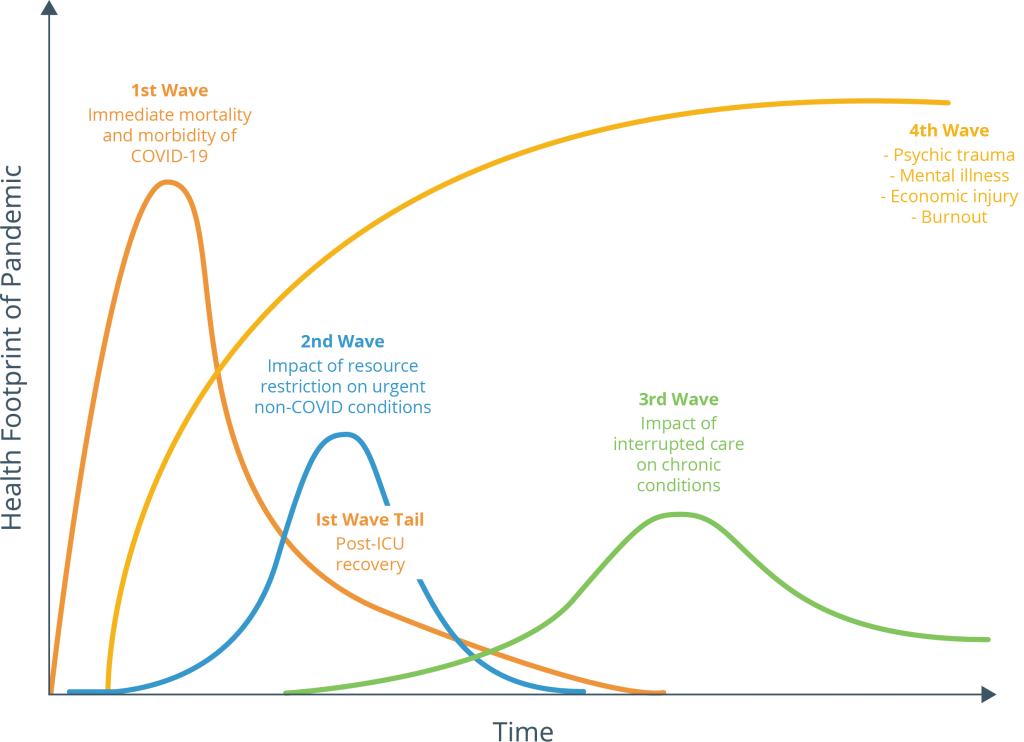
Mental health: the pandemic's fourth wave
US physician Victor Tseng sees mental health as the fourth wave of COVID-19, after mortality, resource restriction and lack of immediate care.
See CCIWA's coverage of the issue here.
Psychological hazards arising from COVID-19 include:
- concern about exposure to COVID-19 at work;
- poor management of OSH risks, lack of equipment and resources such as insufficient appropriate PPE; and
- exposure to poor conditions such as heat, cold or noise in temporary workplaces.
- increased work-related violence, aggression and incivility from patients, customers and members of the public;
- serious illness or death of colleagues or clients e.g. nursing home deaths due to COVID-19;
- racism, discrimination or stigma stemming from COVID-19; and
- self-isolation as a result of suspected workplace exposure.
- increased workloads e.g. supermarket home delivery drivers doing more deliveries and longer hours;
- increased time at work e.g. additional shifts as production moves 24/7 to meet increased demands;
- increased workload e.g. because of increased cleaning requirements or reduction of workers in workplace due to physical distancing requirements; and
- work required to adjust to rapid change e.g. buying new equipment or setting up new procedures.
- working from home or isolation from others due to physical distancing or isolation requirements results in feelings of not being supported;
- reduction in number of workers at workplace completing physical tasks to maintain physical distancing requirements; and
- failure (perceived or real) of employers not implementing new policies and procedure to address new working arrangements.
- increased risk of workplace bullying, aggression and harassment as pandemic continues;
- workplace racism, discrimination or stigma, including towards those who have had COVID-19 or are perceived to be a greater risk to others;
- deterioration of workplace relationships as competing demands lead to less regular and effective two-way communication; and
- decreased opportunity for workplace social connections and interactions.
- lack of planning as a result of the pace of the pandemic;
- continual restructures to address the effects of COVID-19 and a corresponding failure to provide information and training, consult and communicate with or support workers (e.g. manufacturing companies making different products or redeploying staff to meet changes in demand); and
- insufficient consideration of the potential WHS and performance impacts due to COVID-19.
- limitations on workers offering the same assistance to colleagues or clients they normally would or witnessing others’ distress in situations where they can’t access their normal services or support e.g. a cancer ward in a hospital has restricted visitors to reduce the risk to patients. The nurses see their patients and family struggle with this isolation.
Strategies for managing psychosocial risks from COVID-19
- Regularly check in with your workers on how they are going and if anything is stressing them.
- Where workers are distressed about the challenging conditions caused by the pandemic, acknowledge their feelings about the situation and reassure them they are doing what they can in the circumstances.
- Stay informed with information from official sources and regularly communicate or share this information with workers.
- Consult your workers and representatives on any risks to their psychological health and physical health and safety.
- Support innovations to address the psychosocial risks where you reasonably can.
- Provide workers with a point of contact to discuss their concerns.
- Make workplace information available in a central place.
- Inform workers about their entitlements if they become unfit for work or have caring responsibilities.
- Inform workers about their rights under OSH laws, including the right to stop work in certain circumstances and the right not to be discriminated against or disadvantaged for raising health and safety concerns in the workplace.
- Proactively support workers who you identify to be more at risk of workplace psychological injury (e.g. frontline workers or those working from home).
- Refer workers to appropriate work-related mental health and wellbeing support services, such as employee assistance programs or the Coronavirus Mental Wellbeing Support Service.
My staff are working from home. How do I look after their mental health?
The duties under the model OSH laws apply to all workplaces, including when a worker is working from home.
Work-related stress can also occur when working from home, but the controls you put in place may need adjusting (e.g. you might replace a regular staff morning tea, with a weekly email update or videoconference to keep people connected).
Where workers are working from home you should consider the tasks you have asked workers to perform from home and whether doing these in relative isolation could cause stress, and what you can do to minimise that stress.
Before you implement any control measures for working from home, you must consult your staff about how they are feeling, if they are stressed what you can do to minimise that stress.
For those working from home, it might be particularly helpful to consult individually, although that may not always be possible.
What is essential, though, is that there is regular and meaningful communication with your staff, including by telephone and videoconference where possible.
You should also make sure they know who to talk to if they need additional support or are feeling concerned.
For advice and guidance on work, health and safety matters contact CCIWA’s Employee Relations Advice Centre on (08) 9365 7660 or email [email protected].